Spinal Fusion
For people considering spinal fusion surgery, it’s important to understand all the details before deciding. Many people feel overwhelmed when faced with such a big decision, but understanding what goes into having spine fusion can help ease some of your worries and give you the knowledge needed to make an informed choice. We’ll cover everything about spinal fusion: from who it benefits most to recovery time.
If you wish to learn more about spinal fusion, contact Sforzo | Dillingham | Stewart Orthopedics + Sports Medicine at 941.378.5100. Our fellowship-trained physicians will assist you in completely understanding spinal fusion surgery and determining whether this is the best option.
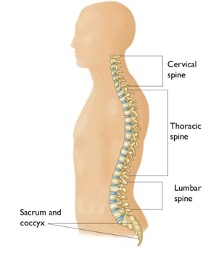
Spinal fusion is a surgical process designed to address issues with the vertebrae in the spine. Fusing two or more of these bones can heal into one solid bone – eliminating any painful movement and restoring stability to your back. In other words, it’s like welding your spine.
Before spine surgery is even considered, your doctor must be able to localize the source of your pain. To accurately identify that location, they may perform imaging studies like:
- X-Rays
- Computed Tomography (CT) Scans
- Magnetic Resonance Imaging (MRI) Scans
Through spinal fusion, motion between vertebrae is eliminated to put an end to the instability and the discomfort associated with it. This method works especially well when movement in a certain part of the spine causes distress due to arthritis. By removing hypermobility from the afflicted area, pain can be eliminated.
Your orthopedic surgeon may suggest a decompression if you struggle with an isolated nerve issue. This operation entails eliminating bone and unhealthy tissues that compress spinal nerves.
Who Needs Spinal Fusion?
Spinal fusion may be recommended for a broad range of medical issues, such as:
- Degenerative disc disease
- Spinal stenosis
- Spondylolisthesis
- Scoliosis
- Fractures in the spinal column
- Infections of the spine
- Tumors
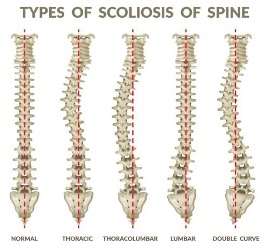
Conservative treatments like medication and physical therapy could be your initial step if you have persistent back pain. However, if those don’t provide the desired results, minimally invasive spinal fusion could be an option for you.
How To Prepare For Spinal Fusion?
During the week before your surgery, you may have a few blood tests completed if needed. You must be aware of every aspect of the procedure beforehand; as a result, feel free to ask queries if anything needs to be clarified. Your surgeon wants nothing more than for you to be completely prepared before going into this experience.
As you prepare for surgery, here are a few important considerations:
- Ensure that your ride to and from the surgery center is arranged.
- Receive clear instructions on any medications – including aspirin or anti-inflammatories – which may be prohibited before and after the surgery.
- Determine if there is anything else off-limits regarding food and drink before your procedure begins.
- Gather essential items such as raised toilet seats, shower chairs with slip-on shoes, and other aids for added safety after returning home post-surgery.
The Procedure of Spinal Fusion
While the patient is unconscious due to general anesthesia, surgeons perform spinal fusion surgery in various ways. Depending on the bones being fused, the location of those bones along the spine, the purpose for fusing them, and potentially overall health and body shape – this technique may vary from person to person. Thanks to modern advancements in medical technology, spinal fusion can be made possible with minimal disruption.
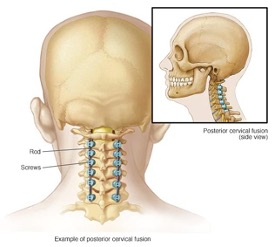
Typically, this process includes the following steps:
- Gaining access to the fused bones, a surgeon will make incisions in one of three areas. When approaching from behind, they may cut into either the neck or back directly over the top of the spine or on its left and right sides. Alternatively, if accessing the spine from the front is preferred, an incision can be made in the stomach or throat area.
- Bone grafts can be acquired from a bone bank or the patient, usually via the pelvis. In some cases, surgeons opt to use artificial materials instead of natural sources. For operations that involve retrieving bones from patients, the surgeon will make an incision close to their pelvic bone before extracting a small portion and stitching up the cut afterward.
- To join the vertebrae, a surgeon inserts a bone graft between them. They might also use metal plates, screws, or rods to keep the bones in place while the graft heals.
Risks of Spinal Fusion
Taken together all major complications from spine surgery are rare and many techniques are utilized to minimize risks. However, some risks include:
- Blood Clots – An uncommon yet serious issue is the formation of blood clots in the legs that can become life-threatening if they break off and travel to the lungs.
- Bleeding – Although some blood loss is expected, it usually isn’t abundant. Donating your blood before a spinal fusion procedure is not necessary.
- Infection – Individuals run the chance of contracting an infection. Medical professionals frequently give patients antibiotics to lower the chance of infection after surgery.
- Spinal Fluid Leak – If this were to occur, the leak is usually repaired and sealed off at the time of surgery. There may be a day or two of bed rest before rehabilitation. Rarely does this lead to any long-term problems.
- Recurring Symptoms – If you are experiencing a resurgence of your initial symptoms, it is likely due to several causes. To ensure your health and safety, inform your doctor immediately so that the proper diagnosis can occur.
- Nerve Damage – Although rare, some operations may cause nerve or blood vessel damage.
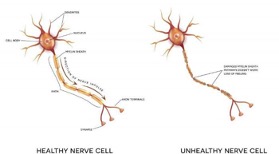
- Pain – Although rare, some patients may experience lingering discomfort in the area.
- Pseudarthrosis – Pseudarthrosis is a condition in which there is an insufficient amount of bone formation for a successful fusion. If you move too soon before the bones can start fusing, pseudarthrosis could be the result – necessitating another surgery.
Spinal Fusion – Recovery
It may be necessary for you to stay in the hospital following the surgery. The duration of that stay is affected by several factors, such as your overall health and existing medical conditions. For many procedures, the hospital stay is quite short.
While during this procedure, you’ll be connected to machinery that continuously tracks your heart rate and regulates your body. You will also have numerous tubes affixed to you for the duration of the operation.
- One IV will be inserted into your arm to provide fluids, antibiotics, and occasional pain medications.
- As an additional measure to help with your recovery, a catheter will be temporarily attached to the area where urine leaves your body. This tube allows you to stay in bed overnight without getting up and going to the restroom. Although it may feel unpleasant or unnoticeable for some people, staying still is key for allowing the time needed to heal your back properly.
It’s important to know that the healing process after back surgery can take six months to one year. The good news is that your spine will eventually heal with commitment and hard work. You’ll be encouraged by your medical professional to stick with physical therapy for however long they deem necessary; this could mean attending appointments weekly or even bi-weekly until further notice. To protect yourself during these first six months of healing, remember these simple life hacks:
- Refrain from twisting motions
- Bending over too far away (especially if lifting)
- Carrying anything overly heavy
If you struggle with spinal issues, wrist pain, or sports-related injuries, contact the Sforzo | Dillingham | Stewart Orthopedics + Sports Medicine team. Our specialists will be delighted to provide a consultation tailored to your needs.